Is addressing multimorbidity the key to improving patient and carer wellbeing?
Multimorbidity means living with multiple chronic physical and mental health conditions. For example, if a patient suffers from anxiety, high blood pressure, and arthritis, they suffer from multimorbidity. Multimorbidity is extremely common in seniors, in fact, 75% of people over 65 are multimorbid, making it a pressing global health challenge.
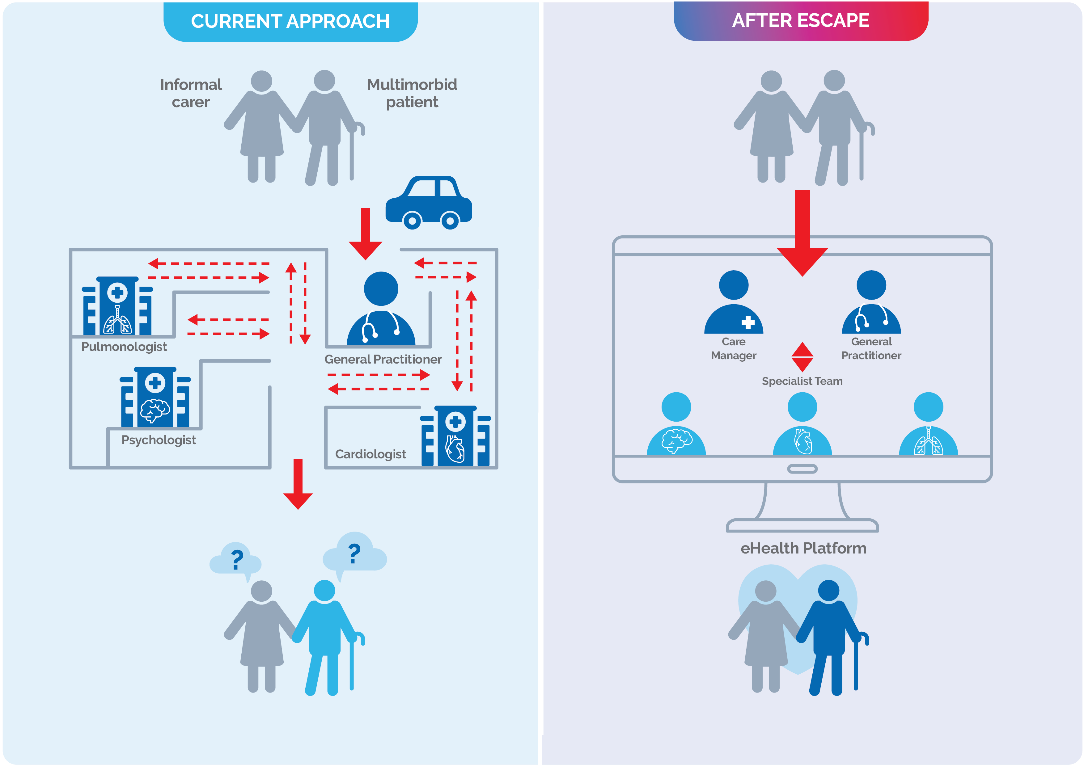
Multimorbidity complicates care for patients and carers as several needs require simultaneous management. From visits to the GP, cardiologist, physical therapy and picking up medications, multimorbid patients have complex needs. Since our healthcare systems are organised around diseases or body parts, and not around the patient, healthcare professionals are often unaware of a patients’ various conditions, unless this information is actively shared. This makes it the patients’ responsibility, or in many cases, the responsibility of the informal carers (i.e., their children or spouse) to manage these appointments and medications.
In particular situations, medications prescribed by healthcare professionals for differing conditions can have serious consequences for patients. When taking two or more medications simultaneously, the drugs can become less effective or pose more serious issues – this is called a drug-drug interaction. Moreover, managing multiple doctors and appointments can lead to delays for necessary treatments. Not only will this affect a patient’s wellbeing and prognosis, but ineffective and delayed treatment is also expensive. Delays in care and adverse drug interactions are just some of the reasons why we need a holistic and integrated approach to managing multimorbid patients.
ESCAPE is an EU funded research project tackling this precise challenge through the utilisation of digital health technologies and a dedicated staff creating personalised treatment plans for patients. As shown in the Figure, ESCAPE employs Care Managers to act as liaisons between the patient and carer, and their various doctors to create a more holistic and patient-centred approach to managing multimorbidity.
ESCAPE’s approach is unique in that it is not only evaluating the physical health of the patients, but also their mental health. When patients are diagnosed with physiological conditions, the side effect is often that their mental health worsens due to this extra burden. But current health practices typically do not consider mental and physical health together, which is why is it is a key priority for ESCAPE.
Secondly, ESCAPE is also evaluating how its intervention impacts carers. Carers and their well-being are often overlooked in patient research projects, despite the huge burden they carry. As carers are not necessarily medical professionals, navigating the healthcare system is not always an easy task and can cause immense stress due to the significant responsibility. This burden of care negatively impacts their mental health and overall wellbeing. Healthcare systems need to reduce the responsibility placed on carers and create more holistic solutions for managing multiple diseases. This will not only improve health outcomes and reduce costs, but it will improve the overall well-being of both patients and carers.
ESCAPE’s clinical trial is beginning in Spring 2022 across six EU countries. As the implementation of the ESCAPE approach begins, the team will test and monitor the model on patients and carers, working towards more holistic and integrated solutions for managing multimorbid patient care. To get regular updates on the implementation follow us on Twitter and ResearchGate and subscribe to our mailing list.
This project has received funding from the European Union’s Horizon 2020 research and innovation programme under grant agreement No 945377 (ESCAPE). This output reflects the views of the authors and the European Commission is not responsible for any use that may be made of the information contained therein.