Continence care, the unnecessarily heavy burden for carers across Europe
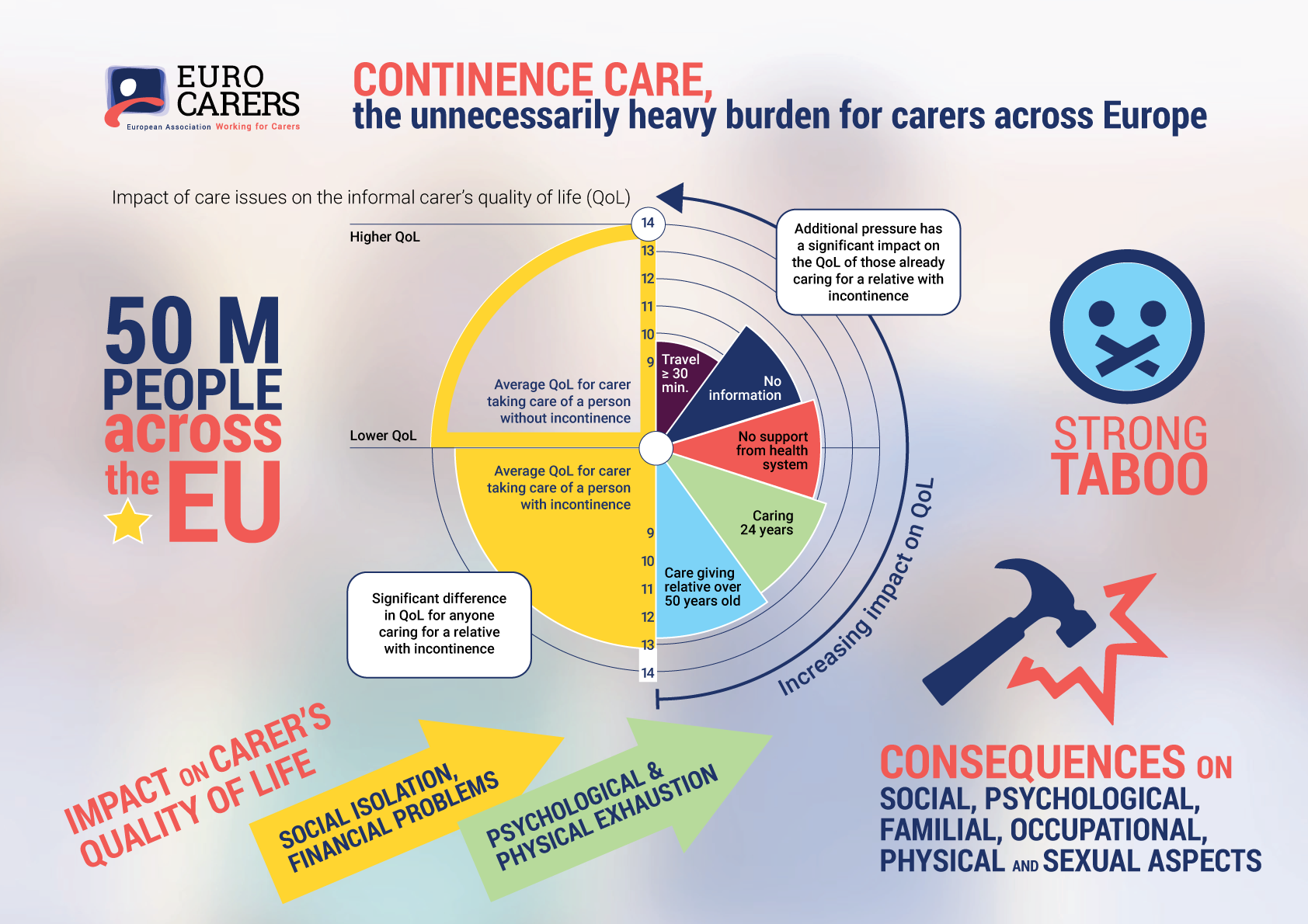
Incontinence is still one of the most strongly tabooed health topics in our societies. Yet, it is a widespread condition which affects 50 million people across the EU and impacts the daily life of more than 15 million informal carers. While it concerns people of all ages, incontinence is particularly common in older age and, with demographic ageing, it is expected that, in a near future, millions more people will see their life change as a result of incontinence. While it is not a life-threatening disease, its symptoms may have serious consequences on social, psychological, familial, occupational, physical and sexual aspects of patients’ lives. When not managed well, the person with incontinence may experience feelings of rejection, social isolation, dependency, loss of control and may also develop problems with their body image. Incontinence also has a remarkably strong effect on carer’s quality of life, as it progressively generates social isolation, financial problems as well as psychological and physical exhaustion.
The importance of person-centred care
The impact of caregiving on informal carers themselves is well documented. Carers are often faced with additional costs as a result of the condition of the person they care for, and their caring responsibilities can be a barrier to entering education and paid employment. The gender dimension of this phenomenon is particularly substantial. Caring can also impact heavily on a carer’s health and wellbeing.
When it comes to incontinence, the lack of appropriate support and the general silence around the topic often aggravate the carer’s experience. Informal carers indeed often find themselves looking for strategies to manage both the care recipient’s loss of autonomy – i.e. their typical informal caregiving responsibilities – as well as their incontinence-related tasks. It is common for carers to try and provide the person with incontinence with opportunities for (self-)controlled excretion, via a routine bladder emptying schedule, for example. While this reduces the number of incontinent episodes and the cleaning up afterwards, it means that the carer and care recipient go together to the bathroom, which may induce shame for both people. Another option consists in relying on home care nurses, but with additional care costs. Finally, when the care recipient becomes totally dependent (including due to incontinence), institutionalisation tends to be the go-to option.
Nevertheless, research shows that, when carers can access appropriate information, count on a strong support network and use suitable incontinence products, they are better equipped to manage incontinence and care tasks in general. It is therefore key to adopt a person-centred care approach focusing not only on the needs of the person with incontinence problems but ensuring that carers have access to appropriate information, adequate support measures and suitable continence care products. Carers enable people with illnesses or disabilities to remain at home and in their own communities safely, independently and with dignity. They are central to the planning, shaping and delivery of services to the people with care needs and in relation to support for themselves. As such, they should be seen as equal partners in care by care professionals who should be better informed and trained about their role, the challenges they face and the added value they bring. Care professionals should provide carers with adequate information about toileting & containment strategies and possible support. They should also give them access to products that facilitate self-management for as long as possible or, when self-management is no longer possible, recommend incontinence product types that are care efficient and easy to use. Too often though, there is a mismatch between individual toileting and containment needs and access to solutions, even when they exist.
The future of toileting and containment care
A lot of progress has been made in the fields of toileting and containment care, especially with regard to self-management. One important aspect is to preserve a healthy skin in an area which is possibly exposed to urine and faeces and for that no rinse skin cleaning & protection products can make a huge difference. Incontinence products like protective underwear, a pant-style product, are very suitable to promote self-management. Belted products, a product type which is easy to apply or remove for highly care dependent persons, can help secure a smooth and efficient delivery of care.
Besides selecting the right product type, absorption level and size that meet a person’s needs, it is important to optimise the care pathway, understand when support with toilet visits and change of pads can best be facilitated, enable a good assessment and improve the delivery of person-centred care. For this, ICT-based solutions offer great potential as they enable an even more targeted delivery of the care to dependent persons. For instance, a recently-developed assessment tool is a digital health technology product that monitors the voiding pattern and the volume of urine lost, providing the base for developing a person-centred toileting and containment care plan. Another approach which utilises digital health technology is a change indicator, which can inform an informal carer or professional that the pad is saturated and need to be changed.
The right policy environment for progress on continence care
From a policy point of view, focused programs and interventions are urgently needed to protect carers, especially those involved in challenging continence care tasks, from feeling overwhelmed and overburdened with care responsibilities, thus maintaining an acceptable level of quality of life. To this aim, preventive measures against the feeling of loneliness and abandonment are needed. For instance, counselling services and self-help groups, wherever possible, with a systematic and early assessment of the carer’s support needs, ideally in conjunction with the multidimensional assessment of the person they care for can prove extremely beneficial.
According to Article 129 of the European Union Treaty, the organisation and delivery of health services and medical care are the responsibility of the Members States. Huge disparities exist between, and within, Member States and these lead to inequalities in how patients are cared for. This can also make it difficult for patients suffering from incontinence to understand their entitlements and to navigate complex bureaucratic reimbursement systems.
In an attempt to take stock of these barriers and formulate recommendations to improve the life of people with incontinence and their carers, Eurocarers took part in a roundtable discussion in 2019, along with AGE Platform Europe, Alzheimer Europe and the European Institute for Women’s Health. This coordination exercise was facilitated by Essity Hygiene and Health AB and its outcomes were captured in a call to action on the provision of person-centred daily continence care, providing broad recommendations on possible ways forward.
These include:
- The need to promote and implement the WHO Guidelines on Integrated Care for Older People;
- The development of assessment practices for people in need of daily support and their carers, thereby allowing the provision of person-centred care;
- The development of continence care-friendly societies based on adapted private homes and public spaces and on the adequate provision of incontinence products to ensure people with incontinence and their informal carers can live a normal and productive life.
To access the call for action, please visit https://eurocarers.org/call-to-action-for-person-centred-daily-continence-care/.
A stronger focus on incontinence management would not only contribute to improving the dignity and quality of life of sufferers, it would help prevent the negative impact of care on millions of informal carers across Europe. The research we have conducted shows that access to appropriate information and suitable incontinence products via user-friendly delivery systems are important stepping stones towards this objective.
Giovanni Lamura – Head of Centre for Socio-Economic Research on Ageing, Italian Institute of Health and Science on Ageing (INRCA), Senior Research at IRCCS